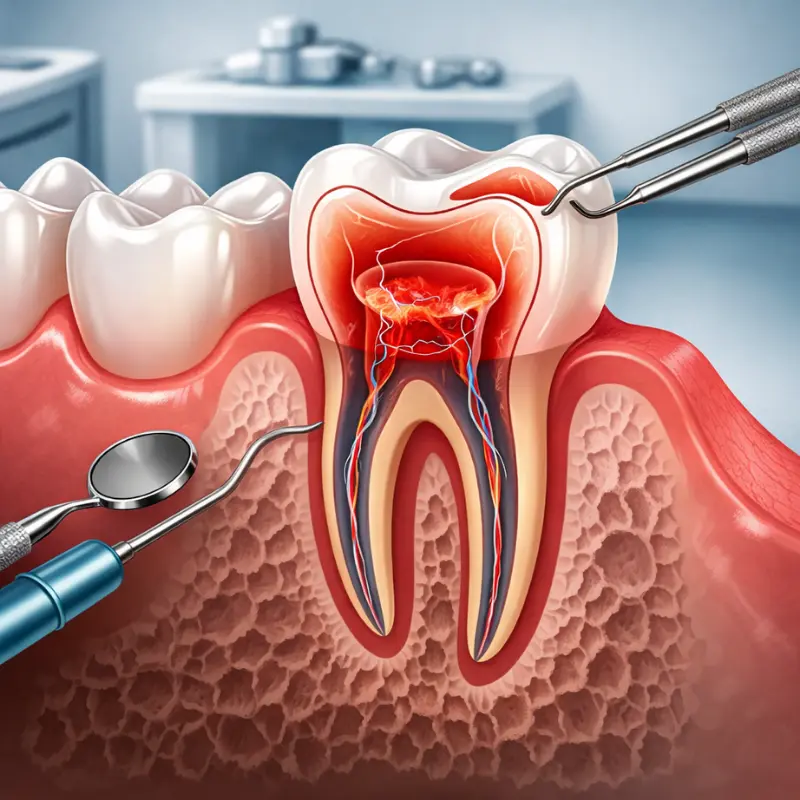
Tooth pain can be confusing, especially when it doesn’t stay in one place. Sometimes, what starts as a simple toothache can seem to move toward the ear or even the jaw and temple. This can feel worrying and may make you think the problem is related to your ear, but in most cases, the source is actually dental.
This happens because the teeth and surrounding areas share nerve pathways. When a tooth is affected by issues like decay, infection, gum problems, or irritation in the jaw joint, the pain can be “referred” to nearby areas. That’s why the discomfort may not always feel like it’s coming from the exact tooth that is affected.
In this article, we will explain why tooth pain can spread to the ear in simple terms, explore the common causes behind it, and help you understand the signs that indicate it’s time to see a dentist for proper evaluation and care.
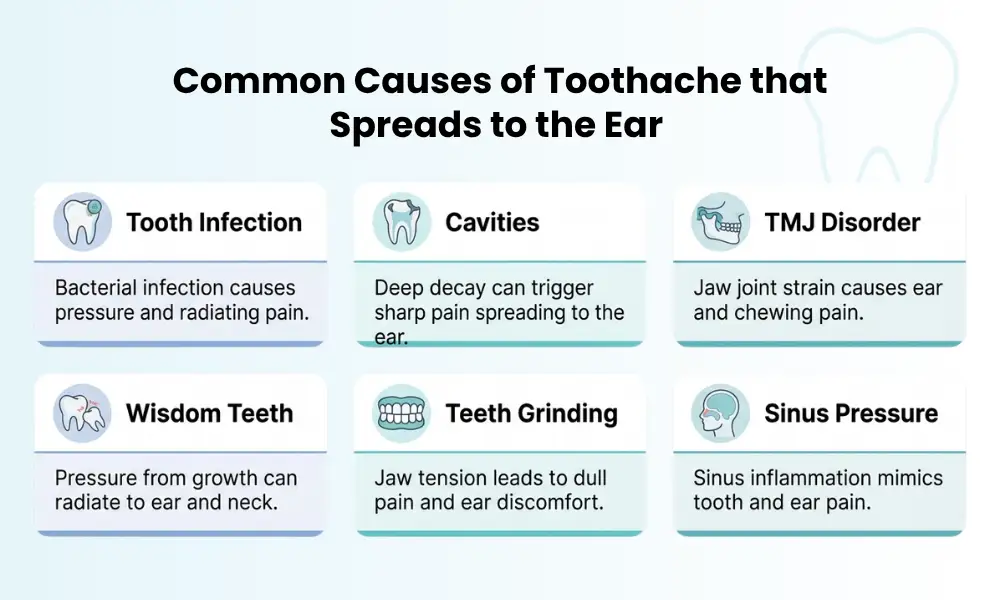
Common Causes of Toothache That Spreads to the Ear
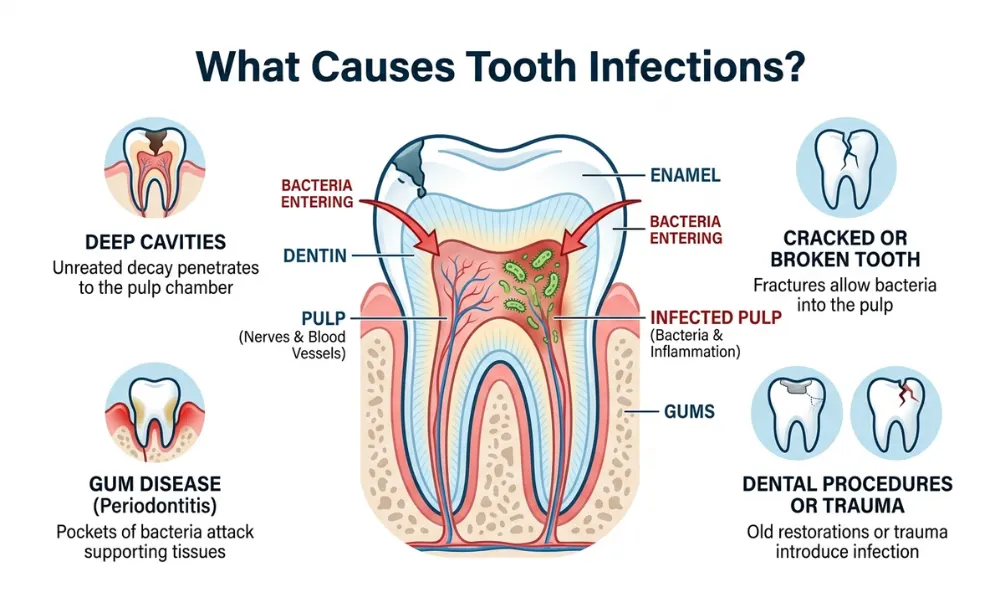
Several dental and jaw-related issues can lead to pain radiating toward the ear.
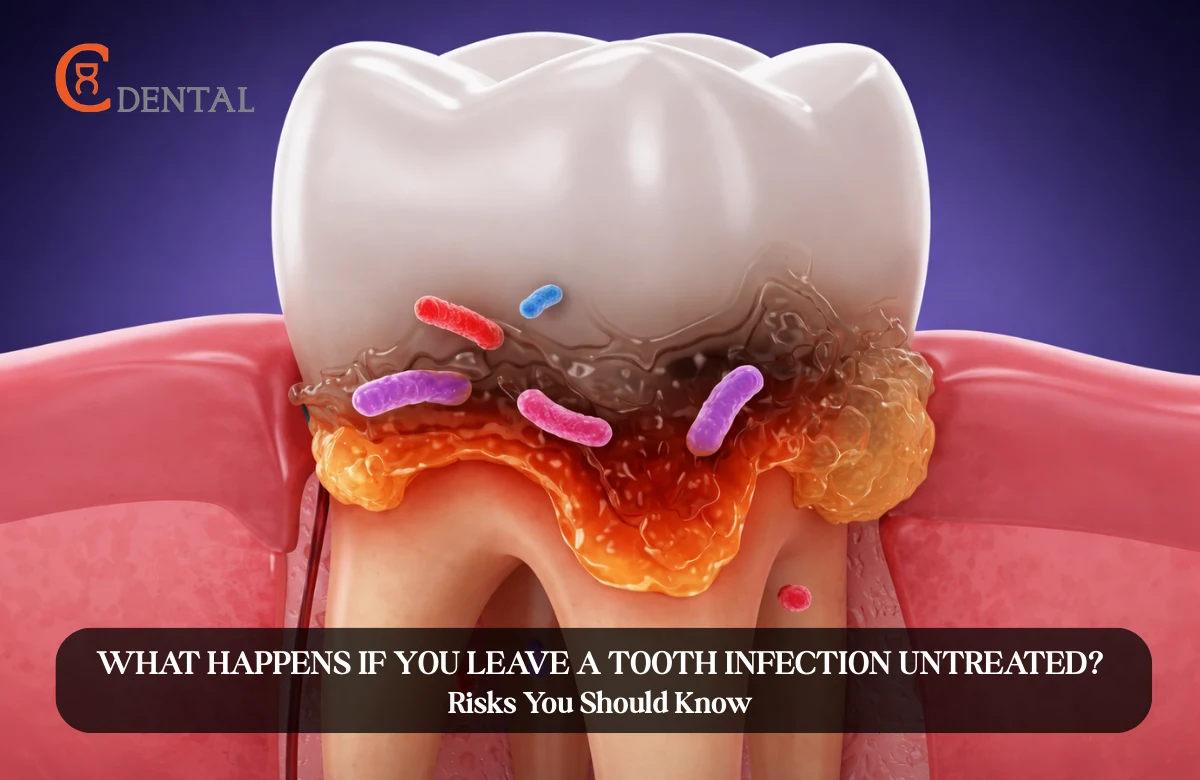
Tooth Infection or Abscess
A tooth infection is one of the most common causes of radiating pain. Bacteria can reach the inner part of the tooth, causing inflammation and pressure. This irritation travels along the nerve pathways and often reaches the ear.
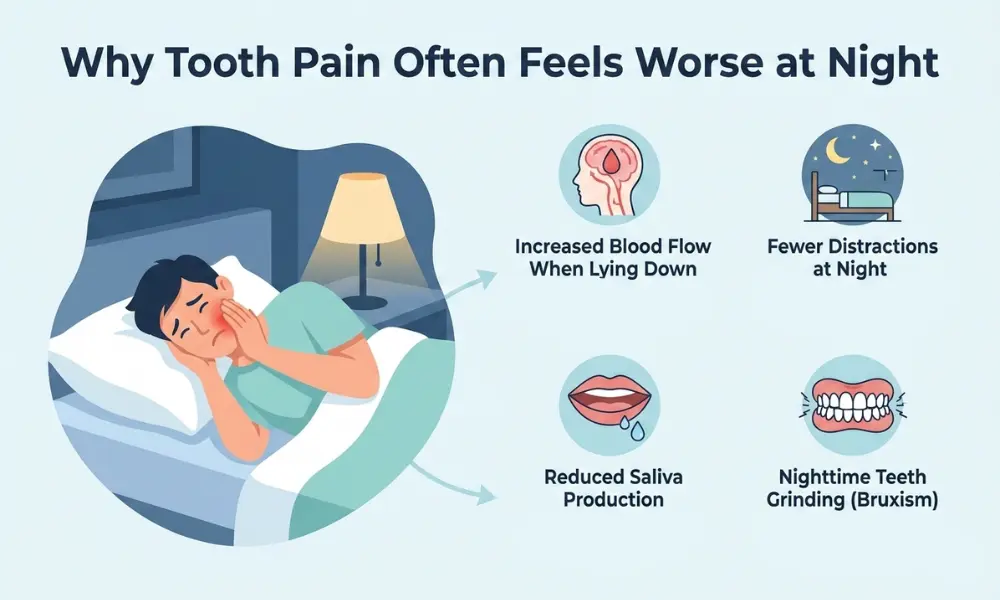
Signs to watch for include throbbing pain, swelling in the gums or face, pain that worsens at night, and a bad taste in the mouth. This condition requires prompt dental attention.
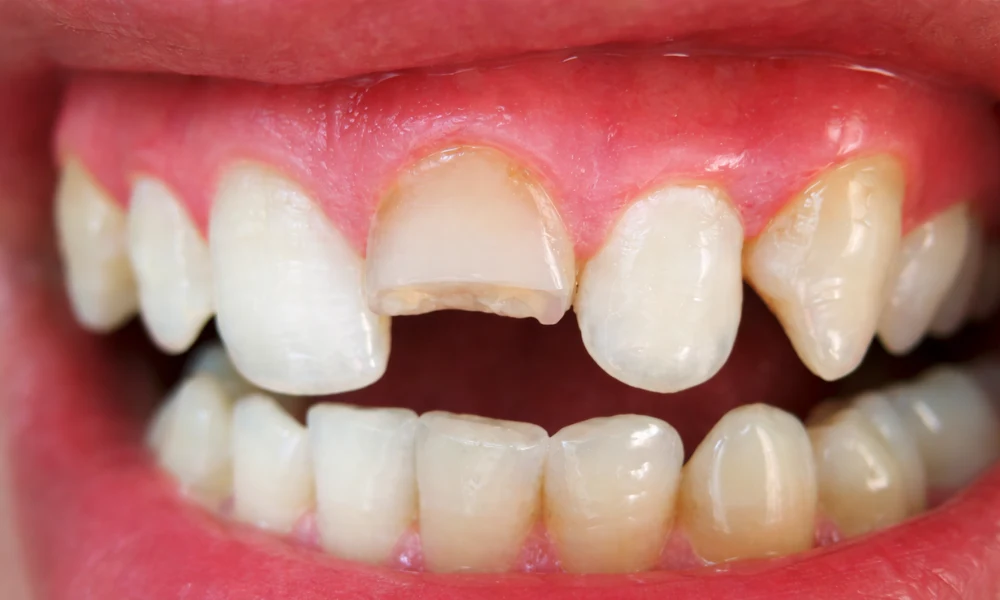
Cavities and Tooth Decay
A cavity can also cause pain that spreads, particularly if it reaches the nerve inside the tooth. Early-stage cavities may cause sensitivity to hot and cold foods, while advanced cavities can produce sharp or shooting pain that extends to the ear.
TMJ Disorder (Jaw Joint Problem)
The temporomandibular joint is located near the ear. Inflammation or strain in this joint can cause jaw pain, ear discomfort, pain while chewing, and sometimes clicking or popping sounds. TMJ-related pain often feels like a combination of a toothache and an earache.
Wisdom Tooth Problems
Impacted or partially erupted wisdom teeth can exert pressure in the jaw, leading to pain that spreads to the ear, neck, and side of the head. This is particularly common in younger adults.
Teeth Grinding (Bruxism)
Grinding or clenching your teeth puts pressure on the jaw muscles and teeth. Over time, this can cause dull tooth pain, jaw tension, ear discomfort, and headaches.
Sinus Pressure
Occasionally, tooth pain is not dental in origin. The upper teeth sit close to the sinuses, so inflammation or pressure in the sinuses can feel like a toothache and sometimes spread toward the ear.
Toothache versus Ear Infection – How to Tell the Difference
Dental pain can often be mistaken for an ear problem. The table below helps differentiate the two:
| Symptom | Tooth Problem | Ear Infection |
| Pain trigger | Chewing, biting | Constant |
| Sensitivity | Hot or cold foods | Not present |
| Fever | Rare | Common |
| Hearing issues | No | Yes |
| Jaw movement effect | Pain increases | No change |
If your pain changes when you chew or move your jaw, it is likely of dental origin.

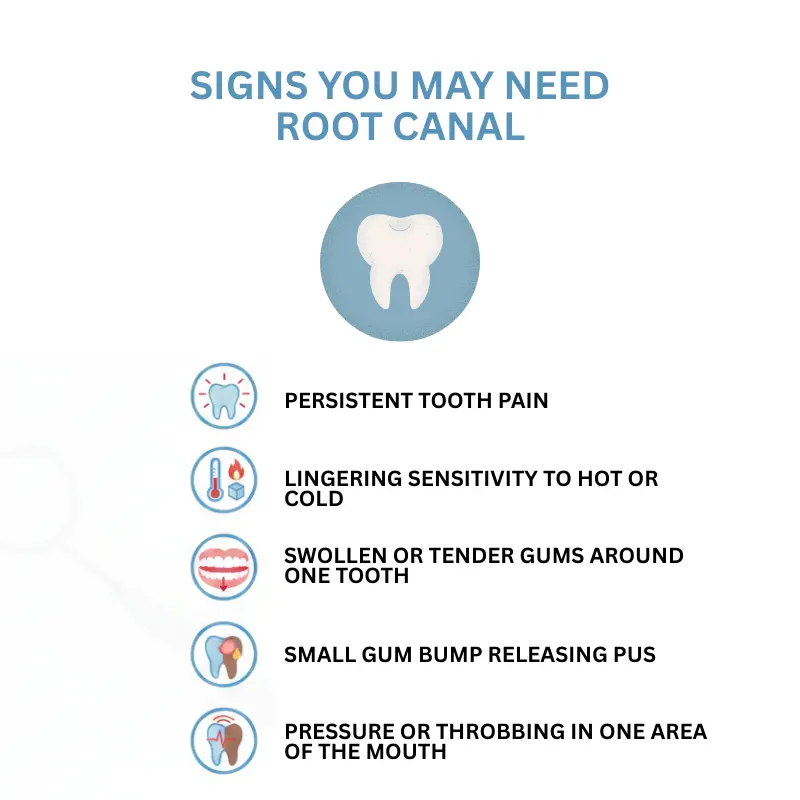
Signs Your Tooth Is Causing Ear Pain
You may be dealing with a dental issue if you notice:
- Pain on one side of your face
- Pain worsens while chewing
- Sensitivity to hot or cold foods or drinks
- Swelling or tenderness in the gums
- Discomfort triggered by jaw movement
These signs strongly suggest that the source of the pain is a tooth or jaw issue, not the ear.
What to Do If Tooth Pain Spreads to Your Ear
While dental treatment is necessary to address the root cause, the following measures can help manage the pain temporarily:
- Rinse your mouth with warm salt water
- Avoid very hot, cold, or sugary foods
- Take over-the-counter pain relief if needed
- Apply a cold compress to the outside of the cheek
These steps help alleviate discomfort but do not treat the underlying problem.
When to See a Dentist Immediately
Seek urgent dental care if you experience:
- Swelling in the face or gums
- Severe or persistent pain
- Fever
- Difficulty opening your mouth
- Signs of infection, such as pus or a bad taste
These could indicate a serious dental problem that requires immediate attention.
How Dentists Treat Tooth Pain That Reaches the Ear
Treatment depends on the underlying cause. Options may include:
- Dental fillings for cavities
- Root canal treatment for infections
- Tooth extraction in severe cases
- Night guards for teeth grinding
- TMJ therapy for jaw-related issues
Once the dental problem is addressed, the ear pain typically resolves as well.
Frequently Asked Questions
A: Toothache spreads to the ear due to shared nerve pathways between the teeth, jaw, and ear. This is known as referred pain, where the brain interprets pain from one area as coming from another nearby region.
A: Yes, in many cases, ear pain is actually linked to dental issues such as tooth infections, cavities, wisdom teeth problems, or TMJ disorders rather than an ear infection itself.
A: If the pain worsens while chewing, biting, or moving your jaw, it is more likely dental. Ear infections are often associated with symptoms like fever, hearing issues, and constant ear pain that does not change with jaw movement
A: In most cases, no. While temporary relief may occur, the underlying dental issue will persist unless treated. It is important to see a dentist to identify and address the root cause.
A: You should consult a dentist if you experience persistent pain, swelling, sensitivity to hot or cold, difficulty chewing, or any signs of infection such as pus, bad taste, or fever. Early treatment helps prevent complications.
Final Thoughts
If your toothache spreads to your ear, it is usually not an ear problem. Pain travels along shared nerve pathways, and your body is signaling a deeper dental issue.
Identifying the cause early and seeking appropriate dental treatment is essential. Addressing the underlying problem promptly will not only relieve the pain but also prevent complications.
If you are experiencing persistent tooth pain, consult a dentist as soon as possible. Early diagnosis and appropriate treatment can not only ease your pain but also protect your long-term oral health.
References
- 5 Causes of Toothache Radiating to the Face– Thomas Dental
- Why Does One Tooth Cause Pain in the Head, Ear, or Neck?– Dr. Sanjay Kalra
- Toothache radiating to the ear – what to do when a toothache spreads to the ear?-Smilesonic.
- When Ear and Jaw Pain Indicate TMD– Colgate
Please subscribe to our social channels for updates related to dental care and oral health.
Instagram: cdental2025
Facebook: CDental
YouTube: C-Dental Clinic